Today, the term “new normal” has worked itself into the common vernacular of most people—but what about the “old normal”? Although it seems like a long time ago, in the not-too-distant past people who became very sick were subjected to a hospital bed until they became better and could finally go home. No alternatives, no exceptions.
There was simply no other way. How could a patient receive hospital-level care anywhere other than… the hospital? How could clinicians achieve the continuous visibility they needed to treat patients’ complex conditions without being under the same roof?
Just as in every other aspect of daily life, healthcare also has a “new normal.” This new normal is marked by a radical rise in the precision and availability of remote monitoring and the broader adoption of virtual care. As remote cardiac telemetry becomes ever-more advanced, we can anticipate an even “newer normal” to take shape—one that will fundamentally transform the structure of the hospital as we know it.
Remote Cardiac Monitoring & the Ever-Changing Normal
It is important to remember that before our “old normal” was an even “older normal.” In fact, telemetric cardiac monitoring was actually introduced far earlier than many people realize. It was first invented in 1949 by Norman J. Holter and began being used for medical purposes in the early 1960s. The first radio-electrocardiograph recording device was actually worn as a backpack and had short transmission capabilities. Eventually, Holter made the it smaller and he and his team sold the patent to an airline equipment firm that manufactured the device for more than 40 years. This was an essential step in advancing the device so that it could eventually be used in clinical environments.
The inception of telemetric monitoring and its evolution since then demonstrates the power of progress in making what was previously impossible, possible. Eventually, remote monitoring in cardiology expanded to include Holter Monitoring, Mobile Cardiac Telemetry (MCT), and Event Monitoring, which can be employed by the clinician for different use cases. InfoBionic’s MoMe™ ARC Platform actually combines all of these technologies in one device, providing the clinician the ultimate freedom to tailor monitoring approaches for each patient’s needs while maintaining full access to patient data.
Of course, today, remote monitoring technologies are a major part of cardiac care and a key diagnostic tool for multi-disciplinary providers. But what if they were more than that? What if they were integrated and applied to fundamentally evolve the structure of the hospital itself?
The Future of Normal & the Fourth Major Hospital Care Unit
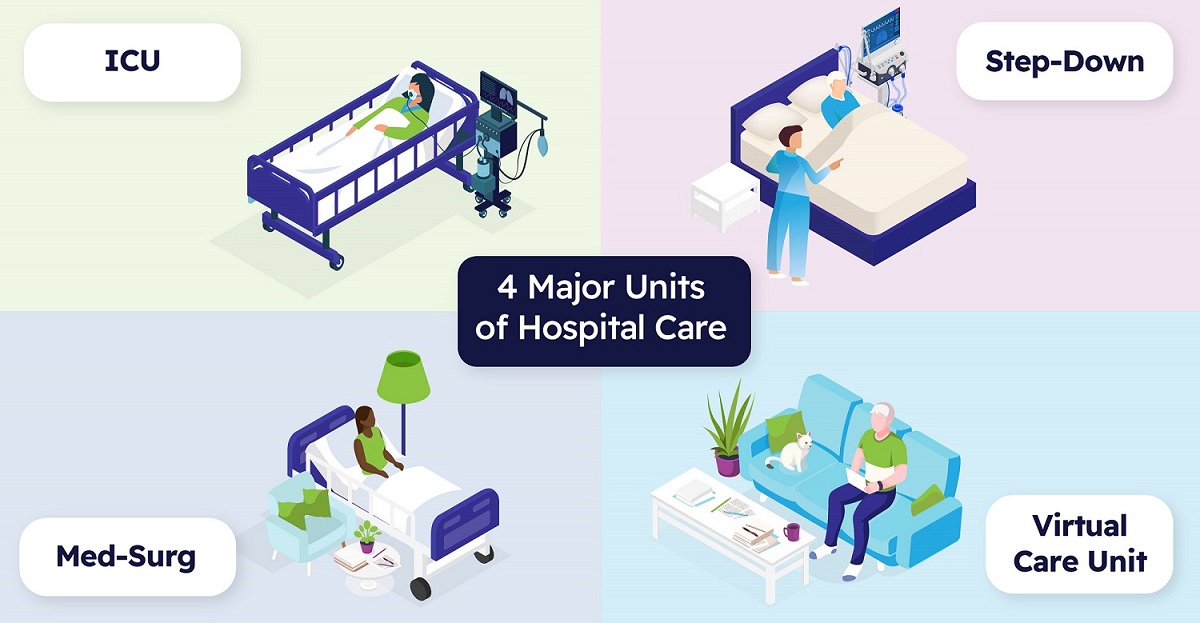
Any clinical professional is well-acquainted with the three major units of the hospital, which are divided based on the level of care acuity that a patient requires. The highest level of acuity is the Intensive Care Unit (ICU), which is marked by continuous monitoring and advanced life support. At a lower level of acuity is the Step-Down unit, which delivers specialized care and continuous monitoring without requiring ICU-level intervention. For patients that require more standard care for non-life-threatening conditions, Meg Surg units and General Medical units provide a regular cadence of monitoring and nursing intervention to ensure a patient continues to recover. All of these units are physically centralized within the hospital, and it is not uncommon that a patient moves from one to the next. No matter the unit, the ultimate aim of the hospital is the recovery of the patient, leading to discharge into their home environment.
As virtual telemetry expands from standard remote monitoring to more advanced monitoring that supports a full range of acuity, it has the capacity to become more than a passive tool but rather, an active part of the hospital itself. What we are seeing is the rise of a fourth major hospital care unit and the very first unit to be physically distributed outside the hospital’s doors. The Virtual Care Unit (VCU) is a virtual extension of the hospital that resides in the comfort of a patient’s home. In addition to freeing hospital capacity from lower-risk patients, the VCU actually extends a hospital’s ability to manage care into areas that were previously ‘blind spots’—the areas that are most likely to drive readmissions and compromise patient outcomes.
Normalizing High-Fidelity Virtual Telemetry with InfoBionic
As the VCU becomes more broadly adopted, the walls of the hospital will expand to include the home. Hospital-to-home care has become even more accessible today, and has been made possible due to the combination of powerful tools and proven technology that the MoMe™ ARC Platform provides.
InfoBionic has embraced the “newer normal” as we’ve dug into the heart of virtual telemetry by creating the MoMe™ ARC Platform. This innovative and revolutionary tool ensures monitoring for any level of acuity in a remote environment, and enables clinicians to gain full power and confidence to step into virtual care, as well as provide patients with the type of care that fits their individual diagnoses and lifestyles.
If you’d like to learn how InfoBionic’s MoMe™ ARC Platform can help you navigate the “newer normal,” contact us today.


